Introduction
Living with sharp, stabbing headaches can feel overwhelming, especially when they stem from a condition like occipital neuralgia, which affects a notable percentage of the population. This type of nerve pain affects not just your body, but also your emotional well-being, making it essential to find the right support. These headaches can make even the simplest tasks feel overwhelming. When traditional treatments don’t provide the relief you need, it’s important to know there are compassionate options available to help you find your way to comfort.
Define Occipital Neuralgia: Understanding the Condition
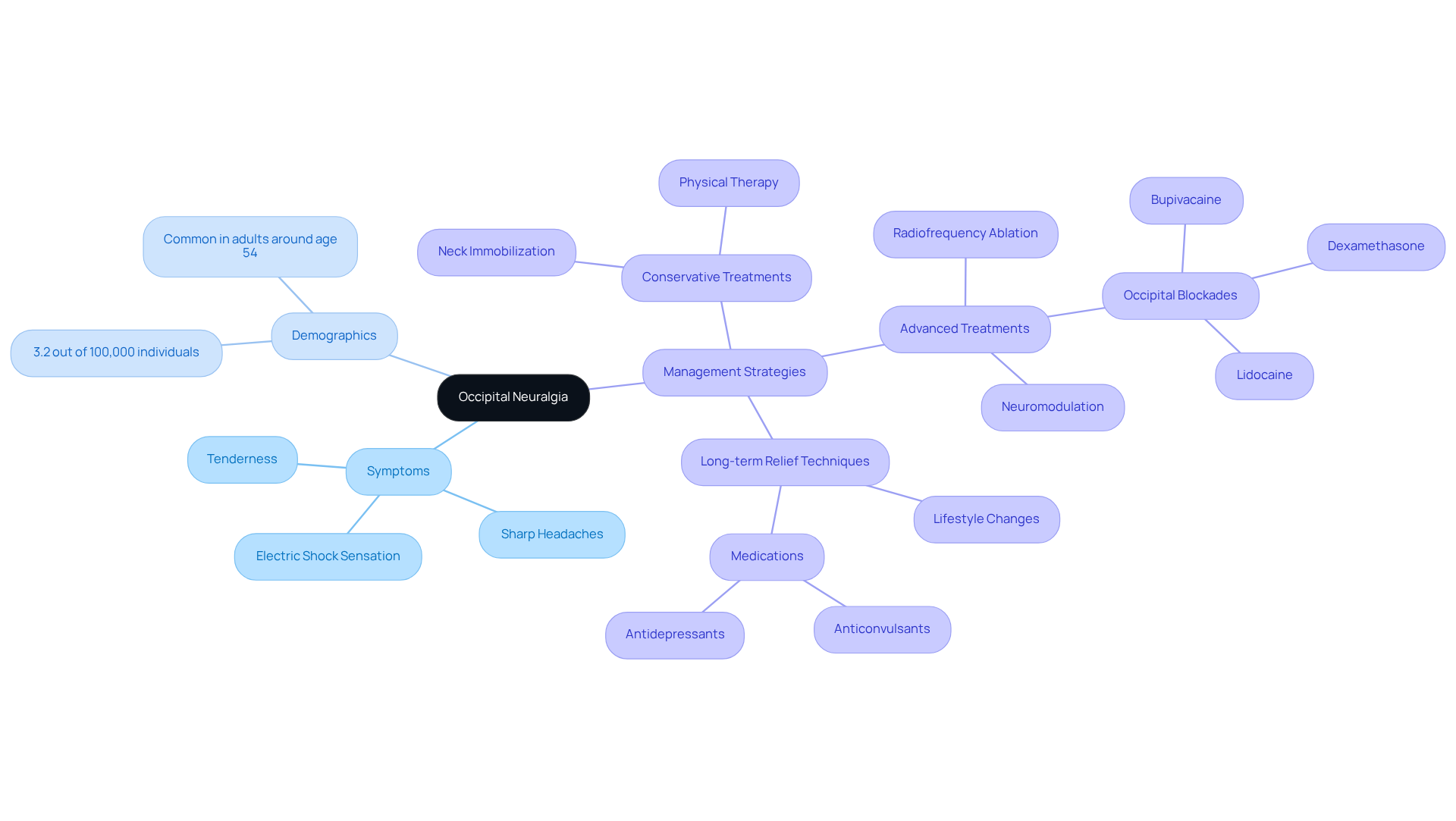
If you’re grappling with sharp, stabbing headaches that seem to come out of nowhere, you’re not alone; many people face the challenges of occipital neuralgia. This type of headache affects many, with about 3.2 out of every 100,000 individuals experiencing it, often striking adults around the age of 54. It’s significantly less common in children, which makes thorough examination essential to rule out other sources of discomfort in the back of the head.
Many people describe their pain as feeling like electric shocks, often starting in the back of the head and sometimes spreading to the forehead, behind the eyes, or even down into the neck. This sudden, severe discomfort can last from seconds to minutes, and it may come with tenderness and altered sensations in the affected area. A positive Tinel’s sign, where tapping along the pathway of the nerve causes discomfort, is often a key indicator of this condition.
We understand that managing this pain can be tough, and it often takes a team of caring professionals to find the right approach for you. Nerve discomfort, or neuropathic pain, can be particularly challenging, leading to distressing sensations like burning or tingling. But with the right support, many individuals can find effective relief.
Management of occipital nerve pain typically involves a blend of conservative and advanced treatment options. While basic interventions like neck immobilization and physical therapy may offer limited relief, more advanced treatments such as occipital blockades with anesthetics like lidocaine and bupivacaine, along with steroids, can provide significant comfort. Many patients experience days or even weeks without headaches after these procedures. Additionally, medications like anticonvulsants and antidepressants, along with lifestyle changes, can enhance overall management. For long-term relief, techniques like radiofrequency ablation (RFA) and neuromodulation may be considered, though they do carry some risks.
Real-world examples show the variability in diagnosis and treatment. In a study of patients with persistent pain after surgery, six out of eight reported complete symptom resolution about five months after receiving block injections. This underscores the importance of accurate diagnosis and personalized treatment plans, as many patients may need multiple interventions each year to maintain relief.
By grasping the complexities of posterior head pain, including its demographics, symptoms, and management strategies, you can take an active role in your treatment. By working together with compassionate healthcare providers, you can navigate this journey toward relief and reclaim the joy in your daily life.
Identify Causes of Occipital Neuralgia: Triggers and Risk Factors
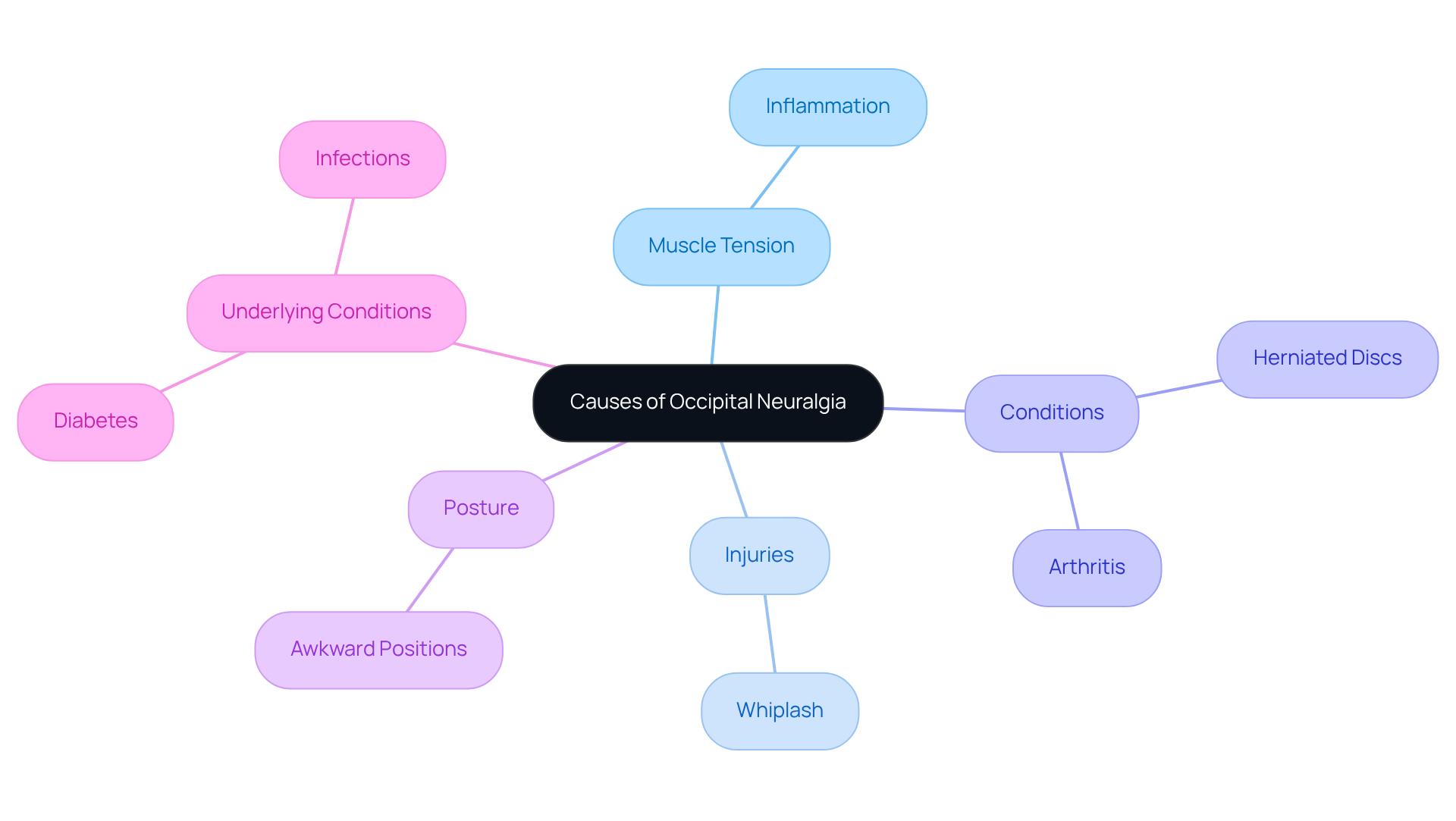
We understand that the causes of occipital nerve pain can feel overwhelming, with various triggers affecting your daily life. Muscle tension, for instance, can lead to inflammation, making your discomfort even harder to bear. That’s why it’s so important to focus on your muscular health.
Injuries, like whiplash, can also play a role, causing damage or inflammation to the nerves in your neck. If you’ve experienced any trauma, it’s essential to take a closer look at your spinal health, as it can make a world of difference in your recovery.
Conditions such as arthritis or herniated discs can cause nerve compression, which may result in occipital nerve pain. We often see how simple changes in posture can bring relief, and our team is here to guide you through those adjustments.
Maintaining awkward positions for long periods can strain your neck muscles and irritate the occipital pathways. Recognizing these underlying factors can truly empower you in your journey toward relief and healing.
Additionally, underlying conditions like diabetes or infections can increase your susceptibility to nerve discomfort. By focusing on muscle tension with personalized therapies, you can take a significant step toward feeling better and reclaiming your life. As one patient, Linda, shared, “Two months after surgery, I am pain-free 90-95% of the time,” highlighting the effectiveness of our approach. Evidence-based alternatives, such as exercise and anti-inflammatory diets, can further enhance your management strategies, emphasizing the compassionate care we provide at Ponte Vedra Spine & Pain Center.
Explore Diagnostic Methods: How Occipital Neuralgia is Identified
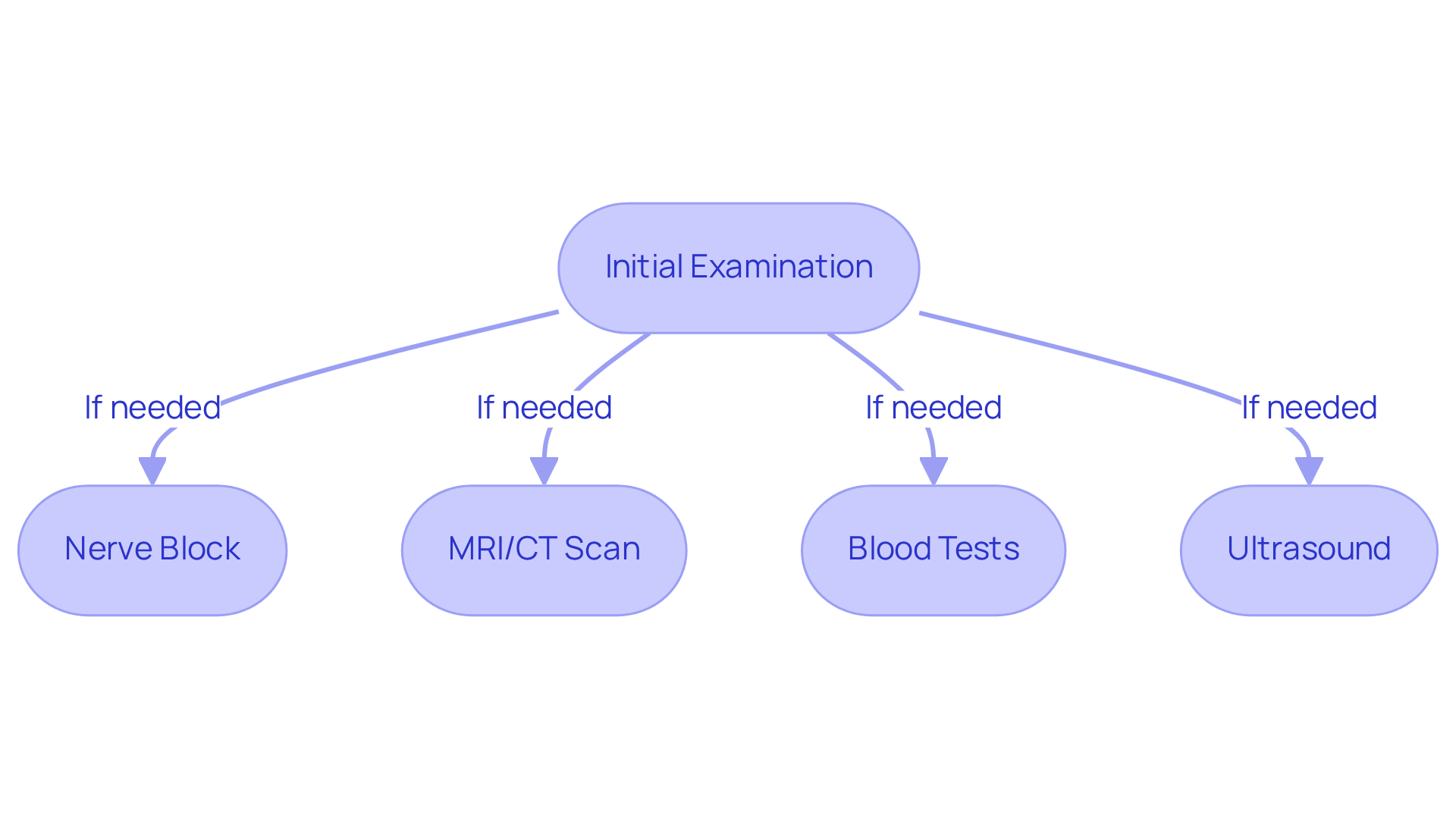
We understand that diagnosing occipital nerve pain can feel overwhelming. It typically starts with a gentle examination to understand your pain better, taking into account your medical history and any factors that might be affecting you. This thorough assessment is essential for identifying the root causes of your discomfort.
If needed, we may use a nerve block to help pinpoint the source of your pain and see if it brings you relief. This step can be reassuring, as it helps us confirm whether the nerve in question is involved in your symptoms.
We might recommend an MRI or CT scan to make sure there are no other issues causing your discomfort, allowing us to focus on the right treatment for you. While it can be concerning, know that occipital nerve pain is often manageable, and we take the time to ensure a thorough diagnosis.
Sometimes, we may suggest blood tests to check for any underlying issues that could be affecting your health and comfort. We can also use ultrasound to take a closer look at the nerves in the back of your head, helping us understand your condition better.
Getting the right diagnosis is essential, and we’re here to guide you through every step of the process. If we find that non-surgical options aren’t effective, we’ll discuss other treatments, including nerve stimulation, to ensure you have the best care possible.
Review Treatment Options: Managing Occipital Neuralgia Effectively
Living with neuralgia can feel isolating and overwhelming, but there are compassionate approaches tailored just for you. Here are some key components of a supportive treatment plan that can help you find relief:
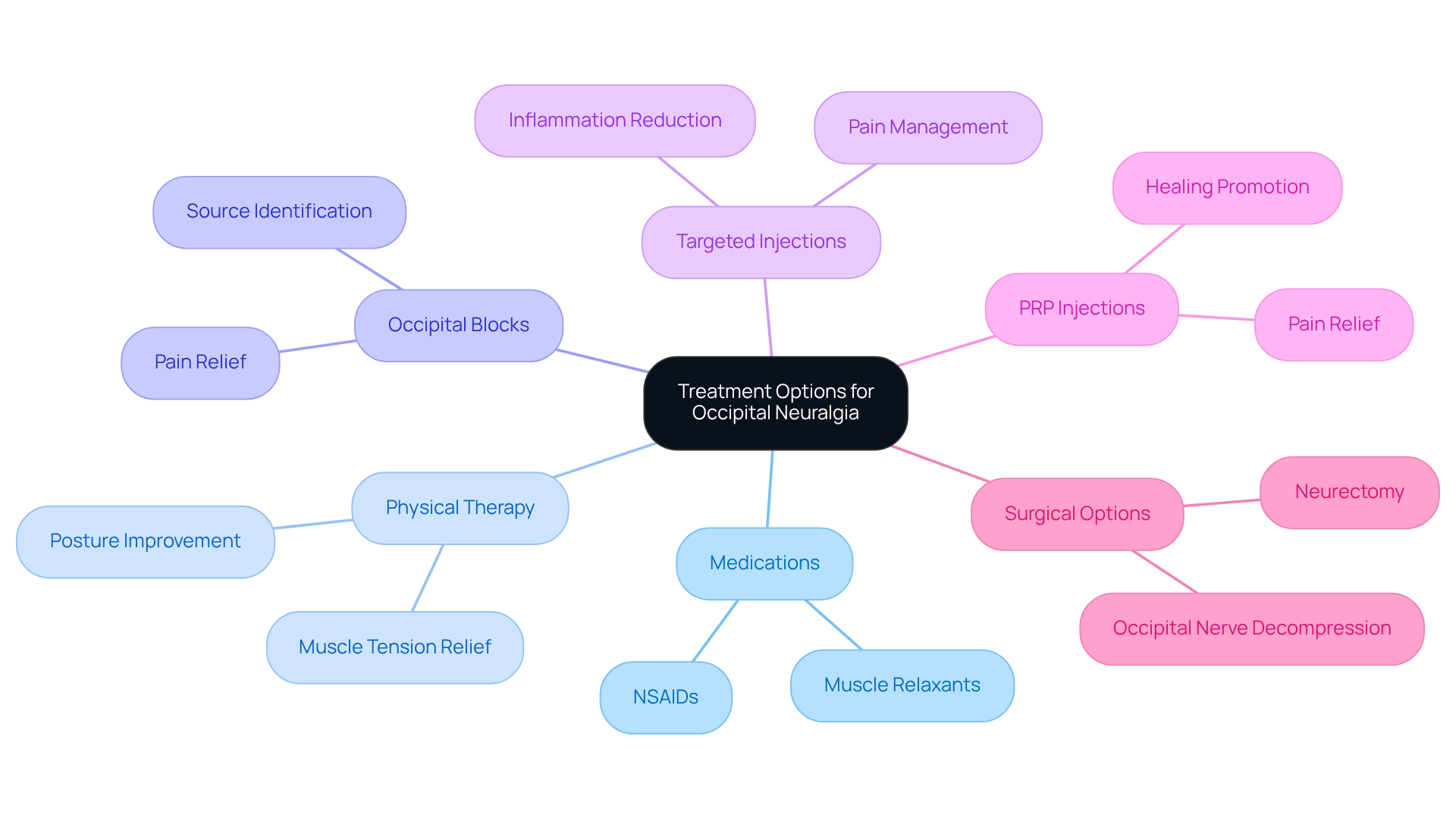
- Medications can play a vital role in your journey to relief. Options like nonsteroidal anti-inflammatory drugs (NSAIDs) and muscle relaxants can help ease your pain and inflammation.
- Physical therapy can be a gentle yet effective way to ease muscle tension and improve your posture, helping you feel more comfortable in your body.
- Occipital blocks can provide both relief and clarity in your treatment journey for occipital nerve pain, helping to pinpoint the source of your discomfort while offering immediate relief.
- In addition to blocks, targeted injections can provide relief and help reduce inflammation in the areas that hurt the most.
- At Ponte Vedra Spine & Pain Center, we’re excited about new techniques like platelet-rich plasma (PRP) injections that can promote healing and bring you relief.
- If conservative therapies don’t bring the relief you need, we can explore surgical options that may offer a new path to comfort and improved quality of life.
Working together with our specialists at Ponte Vedra Spine & Pain Center, we’ll create a personalized treatment plan that focuses on your unique needs and goals. You’re not alone; many people face this challenge, and understanding it is the first step toward finding relief.
Conclusion
If you’re struggling with occipital nerve pain, know that you’re not alone in this challenging journey. This condition, often marked by sharp, stabbing headaches and discomfort in the back of the head, can disrupt your daily activities, making even simple tasks feel overwhelming. By exploring its causes, diagnostic methods, and treatment options, you can better navigate your path to relief and regain control over your well-being.
The article highlights the multifaceted nature of occipital neuralgia, emphasizing the importance of accurate diagnosis and tailored treatment plans. Key insights include:
- The role of muscle tension, injuries, and underlying health conditions as potential triggers for nerve pain.
- Diagnostic methods, such as nerve blocks and imaging techniques, are essential for pinpointing the source of discomfort.
- A range of treatment options-from conservative therapies to advanced interventional procedures-can provide significant relief.
Managing occipital nerve pain is a journey we take together with you, ensuring you feel supported every step of the way. By understanding the intricacies of this condition and actively engaging in personalized treatment strategies, you can take meaningful steps toward alleviating your pain. Embracing a proactive approach not only enhances your potential for recovery but also fosters a deeper understanding of your health and well-being. By taking these steps, you can reclaim your life from the grip of pain and move toward a brighter, more comfortable future.
Frequently Asked Questions
What is occipital neuralgia?
Occipital neuralgia is a type of headache characterized by sharp, stabbing pain that often feels like electric shocks, typically starting in the back of the head and potentially spreading to the forehead, behind the eyes, or down into the neck.
How common is occipital neuralgia?
Occipital neuralgia affects approximately 3.2 out of every 100,000 individuals, primarily striking adults around the age of 54, while it is significantly less common in children.
What are the symptoms of occipital neuralgia?
Symptoms include sudden, severe pain that can last from seconds to minutes, tenderness, altered sensations in the affected area, and a positive Tinel’s sign, where tapping along the nerve pathway causes discomfort.
How is occipital neuralgia managed?
Management typically involves a combination of conservative treatments like neck immobilization and physical therapy, as well as advanced options such as occipital blockades with anesthetics and steroids. Medications like anticonvulsants and antidepressants, along with lifestyle changes, may also enhance management.
What advanced treatments are available for occipital neuralgia?
Advanced treatments include radiofrequency ablation (RFA) and neuromodulation, which can provide long-term relief but may carry some risks.
How effective are block injections for treating occipital neuralgia?
In a study of patients with persistent pain after surgery, six out of eight reported complete symptom resolution about five months after receiving block injections, highlighting the variability in diagnosis and treatment effectiveness.
What role do healthcare providers play in managing occipital neuralgia?
Compassionate healthcare providers are essential for accurately diagnosing the condition and developing personalized treatment plans, which may require multiple interventions each year to maintain relief.
What should individuals do if they suspect they have occipital neuralgia?
Individuals experiencing symptoms of occipital neuralgia should seek a thorough examination by healthcare professionals to rule out other sources of discomfort and to discuss potential management strategies.
List of Sources
- Define Occipital Neuralgia: Understanding the Condition
- New Surgery Offers Hope for Recurrent Chronic Headache Sufferers (https://advancedreconstruction.com/news-media/new-surgery-recurrent-chronic-headaches)
- Occipital Neuralgia – Child Neurology Foundation (https://childneurologyfoundation.org/disorder/occipital-neuralgia)
- Occipital Neuralgia (https://mdsearchlight.com/migraine-headaches/occipital-neuralgia)
- Peripheral Nerve Stimulation Helps Relieve Occipital Nerve Pain (https://practicalneurology.com/news/peripheral-nerve-stimulation-helps-improve-occipital-nerve-pain/2475283)
- Identify Causes of Occipital Neuralgia: Triggers and Risk Factors
- Epidemiology and clinical features of occipital neuralgia: A systematic review and meta-analysis – PubMed (https://pubmed.ncbi.nlm.nih.gov/40017062)
- Occipital Neuralgia (https://hopkinsmedicine.org/health/conditions-and-diseases/occipital-neuralgia)
- Understanding the Causes of Occipital Neuralgia (https://baltimoreperipheralnervepain.com/library/causes-of-occipital-neuralgia.cfm)
- New Surgery Offers Hope for Recurrent Chronic Headache Sufferers (https://advancedreconstruction.com/news-media/new-surgery-recurrent-chronic-headaches)
- Explore Diagnostic Methods: How Occipital Neuralgia is Identified
- Occipital Neuralgia: Occipital Headache, Symptoms & Treatment (https://my.clevelandclinic.org/health/diseases/23072-occipital-neuralgia)
- Get Occipital Neuralgia Treatment | Cleveland Clinic (https://my.clevelandclinic.org/services/occipital-neuralgia-treatment)
- Occipital neuralgia: Symptoms and treatments – Harvard Health (https://health.harvard.edu/pain/occipital-neuralgia-symptoms-and-treatments)
- Review Treatment Options: Managing Occipital Neuralgia Effectively
- Case Report: Percutaneous Peripheral Nerve Stimulation for the Treatment of Occipital Neuralgia | Published in Orthopedic Reviews (https://orthopedicreviews.openmedicalpublishing.org/article/128100-case-report-percutaneous-peripheral-nerve-stimulation-for-the-treatment-of-occipital-neuralgia)
- Freedom from Daily Headaches: Occipital Neuralgia Surgery (https://headachesurgery.com/freedom-at-last-from-non-stop-daily-headaches-how-occipital-neuralgia-surgery-can-turn-your-life-around)
- Occipital Nerve Stimulation for Refractory Occipital Neuralgia: A Multicenter, Randomized, Controlled Trial [StimO Study] – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12986128)
- Cryoanalgesia for Occipital Neuralgia: A Minimally Invasive Treatment Option (https://epimed.com/news/cryo-for-occipital-neuralgia)
- Effectiveness of treatment of occipital neuralgia using the nerve block technique: a prospective analysis of 44 patients – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6130929)